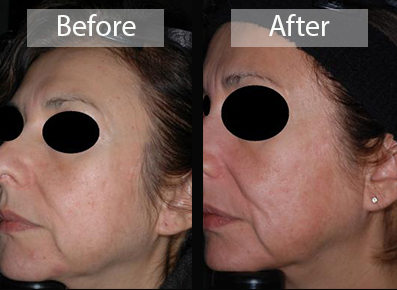
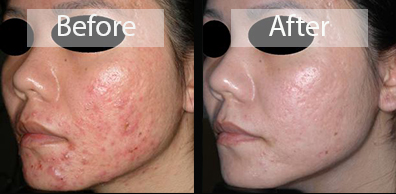
Acne or Acne Vulgaris (as it’s called in the industry) is the most common skin problem encountered in dermatologic practices throughout the world. At our practice, we have served thousands of patients struggling with acne. Our close involvement has even developed into a special academic interest spanning over 60 papers focused on the study of this disease. From benzoyl peroxide treatments to the uses of lasers and light devices – we’ve covered it all! Now, we are pleased to provide you with information on the causes of acne and some of the treatments we offer. Feel free to visit the articles and lectures posted under acne vulgaris and laser reference sections of our website to review our educational activities and investigations into this problem.
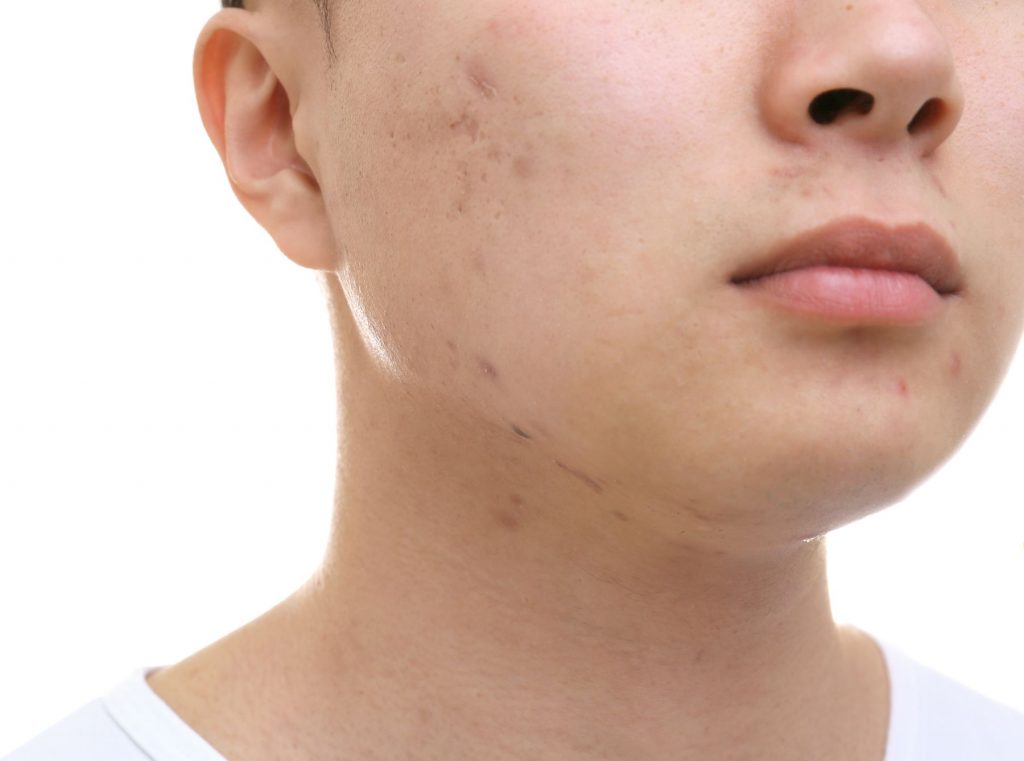
What Causes Acne?
Acne Vulgaris is characterized by an abnormality of the hair follicles on the face, chest, and back. These acne lesions arise from hormonal stimulation of the sebaceous glands associated with the hair follicle. When stimulated, the glands cause an overgrowth of the skin cells lining the ducts. This proliferation and sebum overproduction results in a clogged gland visible as a blackhead or invisible as a micro comedone. There are resident bacteria on the surface of the skin and in the follicle. The primary organism is p-acnes which is an anaerobic bacteria. In other words, this bacteria prefers to grow in the oxygen-deprived environment of the comedone. When this occurs, our body’s immune system steps into action creating an inflamed papule that is also known as a pustule or “zit.” In some instances, there is such an intense inflammation that a large cyst can form. This inflammatory aspect of acne is extremely important to control since it can lead to scarring.
Acne Treatment Options
Benzoyl Peroxide (BPO)
Treating acne involves the use of multiple products in combination to address the key pathophysiologic elements of sebaceous gland hyperactivity, comedone formation, and inflammation elicited by p-acnes.* One of the important cornerstones of acne treatment is benzoyl peroxide also known as BPO.* This impressive product is basically a high oxidizing agent that directly kills p-acnes and does not involve the use of an antibiotic. In fact, chronic use of an antibiotic as a single agent does invariably lead to resistance. However, when used in combination with BPO, resistance is prevented despite continued use of the antibiotic.*
Dr. Tanghetti has been actively imploring the FDA to ban the use of topical antibiotics alone since this can lead to the proliferation of bacteria like MRSA, which are a health care nightmare! We have done many clinical studies with the use of BPO and clindamycin in the treatment of acne vulgaris and found this combination especially effective for acne treatment. Please refer to the chapter we wrote on benzoyl peroxide if you want more information on this product. We have also included an article on resistance in acne vulgaris.
Topical Retinoids
Topical retinoids are another important pillar in the treatment of acne vulgaris.* These treatments normalize skin growth in follicular ducts, thereby permitting the free flow of sebum or oil from the sebaceous glands through the constricted ducts to the surface of the skin. This prevents the over-proliferation of p-acnes and many of the aspects of inflammatory acne characterized by pustules or pimples.* Topical retinoids also have anti-inflammatory properties.* While we use these sometimes as single agents, they are best used in combination with benzoyl peroxide and clindamycin. We have done numerous clinical studies that have demonstrated enhanced efficacy by the use of these combined agents, not only for inflammatory acne but also comedonal-acne.
Schedule OnlineOral Tetracycline Derivatives
There are many instances of moderate to severe acne where topical therapy is just not enough. In those instances, we rely on oral tetracycline derivatives – particularly minocycline and doxycycline. These agents have a direct effect on p-acnes, which is an important part of treating this type of inflammatory acne.* Recent research has also characterized anti-inflammatory properties of tetracycline-like antibiotics on the immune system. It is likely that both mechanisms are important in treating acne vulgaris.* It is not uncommon to use these systemic antibiotics for many months and sometimes years. While we are concerned about bacterial resistance, we are hopeful that the use of benzoyl peroxide and the anti-inflammatory uses of these drugs will prevent this from being a significant problem.* Our goal is always to eventually taper off systemic and topical antibiotics. Topical retinoids are the best for long-term maintenance therapy.*
Accutane
In some cases, particularly those involving cystic acne, topical and systemic therapies are not adequate. However, even in cystic acne, the topical use of BPO and clindamycin with a potent topical retinoid and the systemic use of minocycline is extremely useful.* We have done a clinical study using these agents in combination and have found that with reliable use over three months many cases of cystic acne can be controlled.* In some cases, these agents are not enough and Isotretin, also known as Accutane, is an important part of treatment.* The problems with this drug are well known and include birth defects, mood changes, dryness, acne flares, and other side effects. These issues are controllable and this class of drugs remains an important part of our treatment of severe acne.* It would be important to view the i-pledge program online if you have more questions about the regulatory aspects of this drug.
Spironolactone
Another important patient subset of acne vulgaris are women with adult acne. This can be seen in women who are in their 20s, 30s, 40s, and even 50s. It is often characterized by inflammatory lesions, particularly around the mouth and chin areas. There are often hormonal triggers for adult-onset acne. The drugs listed above are useful as topical agents.* However, topical retinoids are often difficult to use around the mouth due to the over-absorption of topical retinoids causing a drying of the area. BPO/clindamycin and topical dapsone can typically be used effectively in this patient group.* Hormonal therapies, particularly birth control pills with despirdone, do have a place in blocking the effect of testosterone on sebaceous gland overactivity.* If a female is not considering conception spironolactone can also be used. The chronic nature of this condition can be frustrating, but the above therapies can be helpful in the treatment.
Request an Appointment in Sacramento, CA
Dr. Tanghetti’s work has been published in journals such as Lasers in Surgery and Medicine, Journal of Dermatologic Surgery, the Journal of Cosmetic and Laser Therapy, and Cutis. He is a fellow of the American Society for Laser Medicine and Surgery, and a member of the California Medical Association, the American Medical Association, and the American Academy of Dermatology. For a consultation to discuss the acne treatments offered at our clinic, call us at [916] 454.5922 or complete the form below.
Schedule Online
"*" indicates required fields
CLINICAL TRIALS
If you suffer from adult acne, two research studies are being conducted for adult volunteers with acne on the face and/or back.
View Current Trials