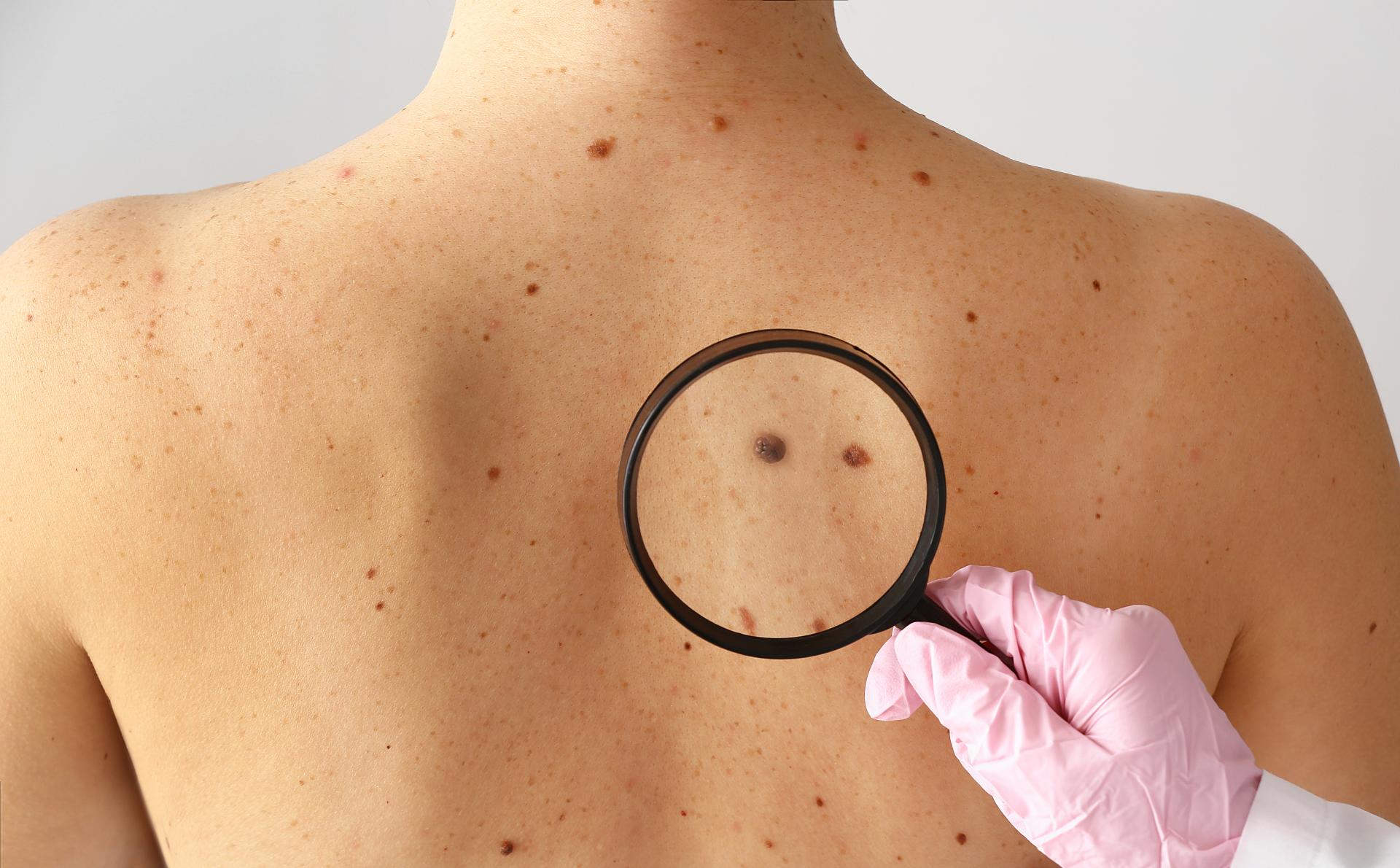
More than 40 percent of all cancers diagnosed and nearly half of all cancer deaths in the U.S. can be attributed to preventable causes, according to the American Association for Cancer Research. This would include excessive sun exposure as it relates to skin cancer.
February is National Cancer Prevention Month, and the focus is on living a healthier lifestyle for cancer prevention. Here are some facts that you should know about skin cancer:
- Skin cancer is America’s most common form of cancer, with over 5 million cases per year diagnosed. Fortunately, it is both preventable and if caught early, manageable.
- 1 in 5 Americans will develop skin cancer by 70.
- The three most common forms of skin cancer include basal cell carcinomas, squamous cell carcinomas, and melanoma respectively. With the latter being on the deadliest forms of skin cancer.
- Having 5 or more sunburns or using tanning beds just a handful of times can double your risk for melanoma.
- Fortunately, when detected early, the 5-year survival rate for melanoma is 99 percent.
“It is a common misconception that skin cancers have associated symptoms, says Amin Esfahani, MD of Golden State Dermatology in Modesto and Merced. “The majority of skin cancers, at their earliest stages, are completely symptom-free. Basal cell cancers can sometimes resemble a pimple or an ingrown hair that persists. Squamous cell cancers can sometimes resemble a rough, dry patch of skin that persists. Since these cancers can be very subtle at their earliest stages, we recommend regularly scheduled skin checks for early detection and treatment.”
What You Can Do to Prevent Skin Cancer
Skin cancers are most frequently caused by too much exposure to ultraviolet (UV) rays. Common sources include the sun, tanning beds, and sunlamps. In the continental U.S., the sun is strongest from 10 a.m. to 4 p.m.
Below are some CDC recommendations for limiting exposure to UV rays and preventing skin cancer:
- Spend more outdoor time in the shade, instead of direct sunlight.
- Keep your legs and arms covered with clothing, preferably those with a UPF rating.
- Wear a hat with at least a 2-inch brim to protect not only your scalp but also your nose and ears.
- Wear UVA and UVB-blocking sunglasses.
- The best sunscreen for skin cancer prevention is one that is broad spectrum (protects against UVA and UVB) with an SPF of at least 30 or higher.
Regular Screenings for Skin Cancer Prevention
The Skin Cancer Foundation recommends annual skin cancer screenings for early detection of skin cancer and growths at the highest risk for transformation into cancer. Golden State Dermatology offers screenings and exam services, as well as a state-of-the-art laboratory where our very own world-class dermatopathologists analyze skin samples with a quick turnaround. An earlier diagnosis assures a timely treatment.
At Golden State Dermatology we offer patient-tailored, state-of-the-art services for the management of skin growths at the highest risk for transformation into cancer. These include liquid nitrogen treatments and blue light therapy, along with other specialized creams and supplements.
However, in the case where cancer is detected, we have skilled dermatological and Mohs surgeons who can effectively treat you in a timely manner. Mohs surgery involves cutting away thin layers of skin in the area where cancer was detected and looking for signs of cancer until there safely are no signs. The goal of Mohs surgery is to remove all of the cancer while sparing as much healthy tissue around it. This is especially recommended in areas of the body that show the most, such as the face and chest. With more Mohs surgeons on our team than ever before, we can provide this service within a reasonable distance from all of our clinics.
Cancer Prevention Awareness All Year Long
While a cancer diagnosis is never good, skin cancer does have an excellent survival rate when caught early. At Golden State Dermatology, we prioritize the health of every patient. We are here to help when it comes to the prevention and treatment of skin cancer.
.